The discussion surrounding “quality of care” in aged care often reveals a tension between two perspectives: that of care recipients, who primarily value outcomes, and that of providers, who focus on the processes that underpin care delivery. Care recipients naturally place great importance on outcomes—whether their health improves, how they feel, and their overall quality of life. Providers, however, often emphasise that true quality of care is rooted in adherence to established care processes, or “best practices,” even when these do not always lead to uniform outcomes.
Theoretical foundations of quality measurement
To fully appreciate the complexity of measuring quality in aged care, it’s helpful to consider Avedis Donabedian’s Structure-Process-Outcome (SPO) framework, which has long been a cornerstone in the field of healthcare quality assessment. According to Donabedian, quality of care can be evaluated across three interconnected domains:
- Structure: The physical and organisational infrastructure within which care is provided, such as staffing levels, facilities, and equipment.
- Process: The methods and practices used in delivering care, including adherence to clinical guidelines and protocols.
- Outcome: The results of the care provided, including improvements in health status, patient satisfaction, and mortality rates.
In aged care, these domains are deeply intertwined. For example, high-quality structures, such as well-trained staff and properly maintained facilities, are essential for supporting the processes that define best practice. However, outcomes, which reflect the end results of care, are often the most visible indicators to care recipients and their families. This framework underscores that quality is multifaceted—focusing solely on one domain, such as process, without considering the others, provides an incomplete picture.
While Donabedian included aspects of patient experience—such as satisfaction—within outcomes, later frameworks sought to give it greater emphasis. In the 1990s, the United States Institute of Medicine (IOM) expanded on his model by introducing additional domains to better capture the complexity of healthcare quality: access and experience. These domains are particularly relevant in the context of aged care:
- Access: Refers to the ability of care recipients to obtain necessary services. While access is often considered at the system level—ensuring that everyone who needs care can receive it—it also plays a critical role in evaluating quality at the provider level. Timeliness in gaining access to a home care package or residential place can be a significant indicator of systemic quality and equity. However, recently concerns have emerged about the decline in access to allied health professionals, particularly in reablement services, following the introduction of mandated nursing minutes. This decline highlights potential gaps in care quality, as comprehensive allied health support is essential for achieving holistic outcomes.
- Experience: Encompasses the care recipient’s personal experience of care, including how they perceive the interactions with care staff, the responsiveness of services, and overall satisfaction with care. Experience metrics, while sometimes bundled with outcomes, offer distinct insights into the effectiveness of care processes and the emotional and psychological impact of care on recipients.
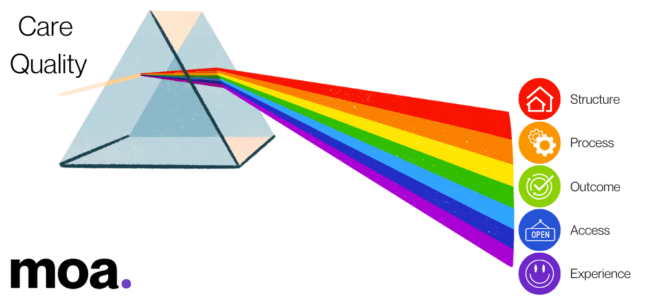
Care quality can be thought about through the prism of five indicator domains
Process vs. outcome: The duality of quality of care
Providers are correct in highlighting that good care practices can lead to different outcomes for different individuals. Factors such as underlying health conditions, genetic differences, and personal circumstances can all influence how care recipients respond to the same treatment. This variability is inherent and sometimes unpredictable, making outcomes alone a challenging metric for evaluating the quality of care. For example, two care recipients might receive identical interventions for managing diabetes, yet experience different levels of blood sugar control due to factors beyond the provider’s control, such as diet adherence or stress levels.
However, this perspective can be problematic when it dismisses outcomes as unreliable indicators of care quality. The paradox lies in the fact that best practices are defined by their proven ability to deliver better outcomes across a population. Research and evidence inform these practices, establishing them as standards precisely because they tend to result in improved health outcomes for most people. If we disregard outcomes as a measure of quality, we risk undermining the foundation upon which these best practices are built.
The role of outcomes in improving care processes
Outcomes, despite their inherent variability, serve as critical indicators of whether care processes are effective. By analysing outcomes at a macro level—comparing them across different care settings or tracking them over time—providers can identify patterns that suggest when a best practice might be underperforming. For instance, if a care home observes an increasing trend in fall-related injuries despite following fall prevention protocols, this might indicate that those protocols need to be reviewed and possibly updated to reflect current best practices.
The complexity of using outcomes as a measure of quality is further compounded by the variability in individual risk factors, which are often beyond the provider’s control. This makes it essential to consider case mix adjustment models that can fairly compare outcomes across different care environments. Without understanding and accounting for this variability, any evaluation of care quality based on outcomes would be incomplete and potentially unfair.
Moreover, best practices themselves are typically derived from research that reflects the average participant in a study. This approach, while useful, may not fully capture the diversity of care recipients in aged care settings today. The generalisability of these practices can be limited, as they may not adequately address the specific needs of different subgroups. For example, pain management guidelines based on studies with younger adults may not fully account for the unique challenges of managing chronic pain in older adults, leading to suboptimal outcomes in aged care settings.
This raises the question of whether it is feasible to design best practices that take into account individual characteristics. While there have been attempts to personalise guidelines based on factors such as age or sex, a truly nuanced approach would require a much deeper understanding of how various individual characteristics influence care outcomes. For instance, adjusting care practices based on a care recipients individual characteristics and comorbidities, rather than using a one-size-fits-all approach, could lead to more tailored and effective care.
Experience and access: Expanding the quality metric
Experience and access are additional dimensions that provide valuable insights into the quality of care in aged care settings. Experience metrics, which capture the subjective perceptions of care recipients, can reveal gaps in the emotional and psychological aspects of care that outcomes alone may not detect. For instance, a care process might be clinically effective but may leave recipients feeling unsupported or disrespected, leading to negative experiences that impact overall satisfaction.
Access, on the other hand, is often a reflection of systemic issues rather than provider-level quality. However, it plays a crucial role in determining who gets the care they need and when. In aged care, delays in accessing services, such as long waiting times for home care packages or residential placements, can severely affect outcomes. The recent decline in access to allied health professionals, due in part to the focus on tracking nursing minutes, is particularly concerning. Allied health services are integral to reablement and overall well-being in aged care settings. Reductions in these services may compromise the holistic care necessary for optimal outcomes. While access metrics may be more suited to evaluating health systems as a whole, they are nonetheless essential for understanding the broader context in which aged care providers operate.
Providers are right to assert that quality care is fundamentally about process. However, this process can only be refined and improved through the ongoing examination and tracking of outcomes and experience, and access. These domains, despite their inherent variability, are indispensable in assessing whether the processes we regard as best practice are indeed serving the needs of care recipients. The relationship between process, outcome, experience, and access is not contradictory but rather a dynamic interplay that drives the continuous improvement of care standards. Through this lens, the measurement of outcomes becomes not a judgment of individual care episodes, but a critical tool in the evolution of best practices, ensuring they remain relevant and effective.



